Illinois and New York have recently enacted legislation permitting physician-assisted death, joining a growing number of states that have embraced this complex and ethically charged practice. This expansion of medical aid in dying, often referred to by various terms such as physician-assisted death, medical aid in dying, doctor-assisted death, or physician-assisted suicide, reflects a significant evolution in American attitudes towards end-of-life choices. While the majority of U.S. states still prohibit physician-assisted death, a recent Pew Research Center survey reveals that a substantial portion of the American populace no longer views the practice as a moral issue, or even considers it morally permissible. This shift in public perception is occurring against a backdrop of increasing legislative action and ongoing societal debate.
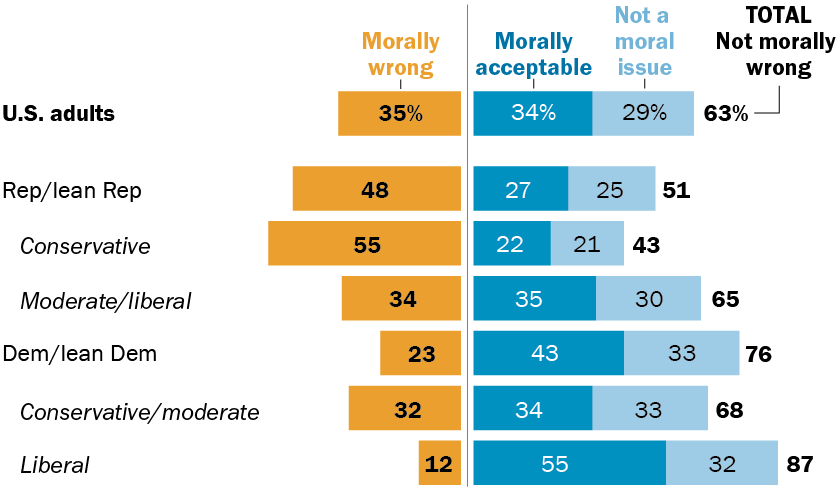
The Pew Research Center’s comprehensive survey, conducted in the spring of 2025, found that approximately six-in-ten Americans hold a permissive or neutral stance on medical aid in dying. Specifically, 34% of respondents indicated that patients choosing to end their lives with a doctor’s assistance is morally acceptable, while an additional 29% stated they do not consider it a moral issue. Conversely, 35% of Americans expressed the view that the practice is morally wrong. These figures underscore a growing societal acceptance, or at least a declining moral objection, to physician-assisted death as a personal choice for individuals facing terminal illnesses.
A Growing Legal Framework for Medical Aid in Dying
The recent legislative victories in Illinois and New York mark a significant expansion of the legal landscape surrounding medical aid in dying. Illinois’ Governor Pritzker’s signing of the bill, following New York Governor Kathy Hochul’s earlier action in February 2026, brings the total number of states and the District of Columbia that permit physician-assisted death to thirteen. This trend, while still representing a minority of states, indicates a discernible momentum towards greater autonomy for terminally ill patients in managing their final moments.
The "Death with Dignity" movement, which gained prominence with Oregon’s passage of its Death with Dignity Act in 1997, has been a driving force behind these legislative changes. The core tenet of these laws is to provide terminally ill individuals with the option to end their suffering through a prescribed course of medication, administered by themselves, under the supervision of a physician. However, the path to legalization has been neither swift nor uncontested, often facing staunch opposition from religious organizations and conservative political groups who argue that such practices violate deeply held moral and ethical principles.

Public Opinion: A Divide Along Political and Religious Lines
While a majority of Americans express a permissive or neutral view on physician-assisted death, this consensus dissolves when examining demographic and ideological divisions. The Pew Research Center’s data highlights a notable divergence in attitudes between Democrats and Republicans.
Political Affiliations and Moral Stances:
- Democrats and Democratic-leaning independents overwhelmingly favor medical aid in dying, with 43% deeming it morally acceptable and an additional 33% viewing it as a moral nonissue. This collective sentiment results in 76% of this group expressing no moral objection.
- Republicans and Republican-leaning individuals present a more divided front. While 27% find the practice morally acceptable and 25% consider it a moral nonissue, a significant 48% of Republicans view physician-assisted death as morally wrong. This stark contrast underscores the politicized nature of the debate.
This partisan divide is further illustrated by ideological subgroups:
- Liberal Democrats are the most supportive, with 55% finding it morally acceptable and 32% considering it a moral nonissue, leading to an impressive 87% with no moral objections.
- Conservative Republicans, conversely, exhibit the strongest opposition. A majority of 55% of this group considers physician-assisted death morally wrong, with only 22% finding it morally acceptable and 21% seeing it as a nonissue.
Religious Beliefs and Moral Frameworks:
Religious affiliation plays a crucial role in shaping views on medical aid in dying. The survey reveals that individuals who are religiously unaffiliated are significantly more likely to support the practice:
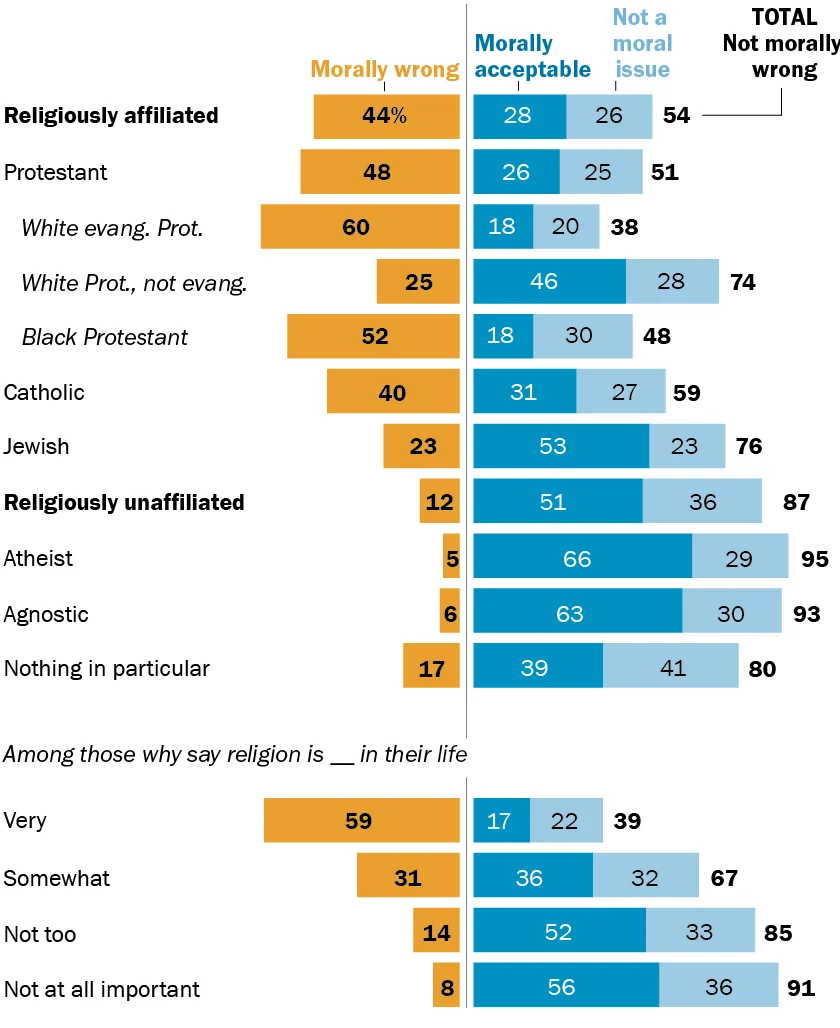
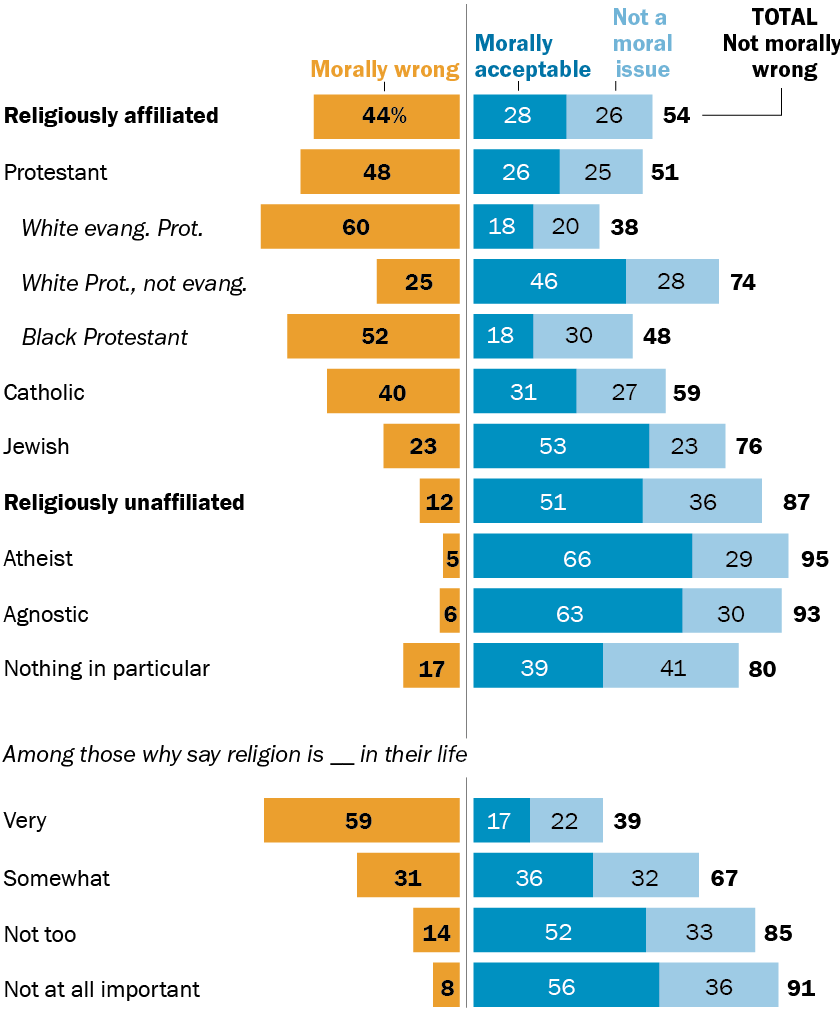
- Religiously unaffiliated adults overwhelmingly express no moral objections, with 51% finding it morally acceptable and 36% considering it a moral nonissue, totaling 87%. This group includes atheists (95% no moral objection) and agnostics (93% no moral objection).
- Catholics show a majority support, with 31% finding it morally acceptable and 27% viewing it as a moral nonissue, totaling 59%. This is notable given that Catholic doctrine, as articulated by the Vatican, prohibits medical assistance in dying.
- Jews also demonstrate strong support, with 53% finding it morally acceptable and 23% considering it a moral nonissue, for a total of 76% with no moral objections.
- Protestants exhibit more varied opinions depending on their specific denomination. While White Protestants who are not evangelical lean towards acceptance (46% morally acceptable, 28% nonissue, totaling 74% with no moral objections), White evangelical Protestants and Black Protestants show higher rates of moral objection.
- White evangelical Protestants are the most likely among religious groups to view the practice as morally wrong, with 60% expressing this view.
- Black Protestants also show significant opposition, with 52% deeming it morally wrong.
The intensity of religious belief also correlates with moral stances. Americans who describe religion as "very important" in their lives are far more likely to consider physician-assisted death morally wrong (59%) compared to those for whom religion is "not too important" (14%) or "not at all important" (8%). This suggests that a deeply ingrained faith can influence perspectives on end-of-life decisions, often aligning with traditional religious teachings that may view human life as sacred and divinely ordained.
Nuances in Terminology and Ethical Considerations
The debate surrounding physician-assisted death is often complicated by the variety of terms used to describe it, each carrying different connotations. The Pew Research Center explicitly surveyed opinions on "patients choosing to end their lives with the help of a doctor," using "physician-assisted death" as a neutral shorthand. However, it acknowledges the politicized nature of the language.
- Physician-assisted suicide: This term is frequently employed by groups that oppose the practice, including the American Medical Association (AMA) in certain contexts, and is often associated with a moral judgment of suicide.
- Medical aid in dying (MAID): This is the preferred term by many proponents and healthcare organizations, emphasizing the medical context and the patient’s autonomy.
- Death with dignity: This phrase, popularized by the advocacy movement, highlights the desire for a peaceful and dignified end to life.
Understanding these terminological distinctions is crucial for interpreting public opinion and legislative debates, as the choice of words can significantly influence perception and emotional response. The AMA, while acknowledging the ethical complexities, has historically maintained a neutral stance on physician-assisted suicide, with individual physicians free to participate or abstain based on their personal conscience.
Historical Context and Ongoing Debates
The legal and ethical discussion surrounding physician-assisted death in the United States has a history stretching back several decades. The late 20th century saw increasing advocacy for patient autonomy in end-of-life care, fueled by high-profile cases and growing awareness of palliative care options.
- 1990s: The landmark case of Dr. Jack Kevorkian brought the issue of physician-assisted suicide to national prominence, sparking intense public and legal debate. Oregon’s passage of the Death with Dignity Act in 1997 was a pivotal moment, establishing the first legal framework for medical aid in dying in the U.S.
- Early 2000s: Following Oregon’s lead, a handful of other states, including California, Washington, Vermont, and Montana, enacted similar legislation or saw court rulings that permitted physician-assisted death under specific conditions.
- 2010s-2020s: The movement continued to gain momentum, with states like Colorado, Maine, New Jersey, Hawaii, and most recently Illinois and New York, passing laws. This period also saw increased legislative efforts in numerous other states, though many faced significant opposition and failed to pass.
The ongoing debates often center on several key ethical considerations:
- Patient Autonomy: The right of individuals to make decisions about their own bodies and lives, especially when facing unbearable suffering from a terminal illness.
- Physician’s Role: The ethical responsibilities of physicians, balancing the duty to preserve life with the imperative to alleviate suffering.
- Vulnerability and Coercion: Concerns that vulnerable individuals, such as the elderly, disabled, or those with mental health conditions, might be coerced or unduly influenced into choosing medical aid in dying.
- The Nature of Suffering: Defining what constitutes "unbearable suffering" and whether it can extend beyond purely physical pain to include psychological and existential distress.
- Religious and Moral Objections: The deeply held beliefs of various religious and ethical traditions that may prohibit or condemn intentionally ending a human life.
Implications and Future Outlook
The trend towards broader legalization of medical aid in dying, coupled with increasing public acceptance, suggests that this will remain a significant and evolving issue in American society. The data from Pew Research Center indicates that the conversation is shifting from a primarily moral debate to one increasingly framed around personal choice and the alleviation of suffering for terminally ill individuals.
The legal framework in states that permit medical aid in dying typically includes stringent safeguards:
- Terminal Prognosis: Patients must be diagnosed with a terminal illness that is expected to result in death within a specified timeframe (e.g., six months).
- Mental Capacity: Individuals must be deemed mentally capable of making an informed decision, free from coercion or undue influence.
- Multiple Requests: Usually, at least two oral requests and one written request for medication are required, separated by a waiting period.
- Physician Consultation: Patients must typically consult with two physicians, one of whom is the attending physician and the other a consulting physician, to confirm the diagnosis and prognosis.
- Self-Administration: The medication must be self-administered by the patient.
As more states consider and enact such legislation, the legal and ethical landscape of end-of-life care in the United States will continue to be reshaped. The findings from Pew Research Center provide a crucial snapshot of public opinion, highlighting both growing consensus and persistent divisions that will undoubtedly fuel future discussions and policy developments. The challenge ahead lies in navigating these complex ethical, religious, and personal considerations while ensuring that the rights and dignity of all individuals, regardless of their beliefs or circumstances, are respected.